Written By: Ogunfeitimi Iyanuoluwa Faith
An elderly man once stopped me during my final-year research project. His eyes held great frustration as he spoke: “You researchers come here, disturb us with your questions, collect your data, and then we never see you again. Nothing changes. Nothing improves.” Here was someone who had given his time. Who had shared his health information and trusted that it would lead to something better.
But the problem isn’t far-fetched. Our systems are broken at multiple levels. There exists a gap between gown and town: knowing and doing, between labour and compensation, between knowledge and impact. The data value chain offers a framework for understanding this breakdown.
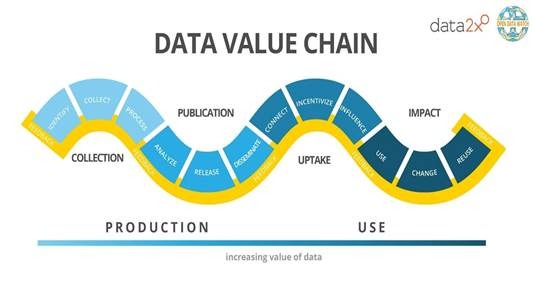
The data value chain explains how data is created and used, starting with the need for recognition of data and ending with its eventual use or reuse for making informed decisions. It describes how data moves through four essential stages: collection, analysis, production, and usage. Data is gathered, analyzed to reveal patterns, transformed into research findings or knowledge products, and finally used to inform decisions and drive change.
Too often, the chain breaks at the third stage. Knowledge gets produced but is never utilized.
Consider the lifecycle of a typical undergraduate and postgraduate thesis: Months of data collection, rigorous analysis, and carefully crafted findings, all in a document that sits on a departmental shelf, gathering dust. The knowledge was created, an existing question has finally been answered; however, it ends on a shelf..
The same pattern repeats in healthcare: patient data are collected, studies are conducted, papers are published in reputable journals, and then… nothing: no real-world application.
This is why Nelson Mandela’s famous declaration that “education is the most powerful weapon which you can use to change the world” now rings hollow to many. The weapon exists, but we have forgotten how to wield it.
From a systems thinking perspective, this reflects a failure in how different parts of the system interact. Researchers, healthcare workers, policymakers, and communities function as interconnected parts of the system, yet knowledge does not flow effectively through them. A functioning system relies on communication, coordination, and feedback between its parts so that evidence produced can shape decisions and practice. When these links are weak, data is generated but impact is lost.
Viewed through a systems thinking lens, the problem is not the absence of data, but the absence of connection. Health systems are not a single structure but a network of interacting parts, each influencing the other. When these relationships are poorly aligned, knowledge remains isolated and interventions fail to achieve their intended effect. Systems thinking therefore shifts attention from isolated outputs, such as published research, to the pathways through which knowledge moves and is applied.
Impact emerges when data becomes part of decision-making. In healthcare, this may involve translating research into clinical guidelines, combining data sets to identify population trends, or using evidence to design and evaluate interventions. Such actions recognize that interventions influence multiple parts of the system and must be guided by an understanding of these interactions.
The use of data depends on strategies that link knowledge producers to knowledge users. Policy briefs, media communication, and community engagement help bridge the gap and strengthen feedback within the system. For students and researchers, the key question remains: must research end on a shelf or stop at publication, or can it inform decisions that translate to tangible impacts? For academic institutions, the challenge is whether they can strengthen the transition from knowledge production to knowledge adoption.
Completing the data value chain is therefore a systemic task that requires strengthening the links between knowledge creation and application. When these links function well, healthcare research becomes a tool for improving services, guiding policy, and advancing equity. When they do not, the system produces knowledge but without change.
The knowledge exists. Now we must use it.
REFERENCE/ACKNOWLEDGEMENT
- Prof. Sunday Olakunle Idowu (Professor of Pharmaceutical Profiling and Informatics, University of Ibadan).
- Open Data Watch (2024, December 9). The data value chain: Executive summary. Open Data Watch. https://opendatawatch.com/reference/the-data-value-chain-executive-summary/
- De Savigny, D., & Adam, T. (Eds.). (2009). Systems thinking for health systems strengthening. Alliance for Health Policy and Systems Research, World Health Organization.